Pregnancy and Childbirth Emergencies
Emergency Childbirth
Your role as a first aider during an emergency childbirth is to help the mother deliver the baby, to protect the mother and baby, and to save all parts of the placenta and amniotic sac until medical help takes over.
If labour is in the second stage, the baby could be born quite soon. Recognize the second stage of labour by the following indications:
- Longer and stronger contractions, less than two minutes apart.
- The mother’s previous experience. If they say the baby is coming, believe them.
- Bulging of the vaginal opening and seeing the baby’s head (called crowning).
- The mother is straining and pushing down, and feels like they have to have a bowel movement.
If you see these signs, you will probably not have time to get the mother to medical help. Call 9-1-1 and get ready to deliver the baby.
Emergency Delivery
The following section describes the stages of an emergency delivery.
Stage 1 – Labour
To give first aid during labour, perform the following steps:
- Locate someone to help you.
- Get the materials you will need to deliver the baby and the placenta:

- First aid kit (obstetrics kit if available)
- Clean towels, blankets
- Tape
- Plastic bag(s)
- Gloves
- Gather the history:
- Length of pregnancy
- Previous births
- Complications during pregnancy
- Medical history (e.g., bleeding disorders, heart/breathing problems, etc.)
Stage 2 – Birth of the baby
During the second stage of labour, when the baby will be born very soon, place the mother on their back with knees bent and head supported. If they prefer another position, use that position. Cover them with sheets so you can easily lift them to check on the progress of labour.
When the head appears, encourage the mother:
- To push with contractions
- Hold their breath while pushing for no more than 7 to 10 seconds
- Place their chin to their chest and avoid arching their back
Place your hand on the top of the baby’s head as it crowns and apply slight pressure with the palm of your gloved hand to prevent an explosive delivery. Support the baby’s head once delivered, keeping the head lower than the body.
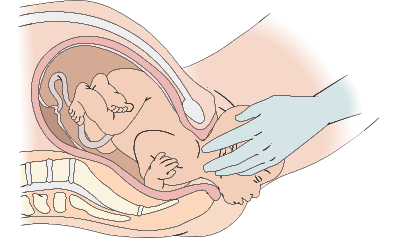
The head will (usually) be face down and then turn to the side to allow the shoulders to deliver. At this point, break the amniotic sac around the baby’s mouth and nose if it has not already broken on its own.
Check for the umbilical cord around the baby’s neck and carefully remove it from around the neck if needed. At this point, have the mother slow down their pushing. Once the shoulders have delivered, the rest of the baby will come out quickly.
A newborn is covered in fluids and is difficult to hold; therefore, ensure you maintain a firm, yet gentle, grip on the newborn.
Stage 3 – After the birth of the baby
The baby should begin to cry (and therefore breathe) on their own, particularly after the amniotic sac has been broken. If this does not happen, stimulate the baby to make them cry by gently flicking the bottom of their feet or rubbing their back. If this does not stimulate the baby to cry within 30 seconds, begin CPR.
Wrap the baby in a clean blanket to maintain their body heat. If the umbilical cord is still pulsating, keep the baby at the same level as the vagina until it stops. If the umbilical cord has stopped pulsating, place the baby on the mother’s chest to help keep the baby warm. Encourage nursing, as this can improve the bond between baby and mother, will help in the delivery of the placenta, and may help decrease bleeding.
| Record the time of the delivery. |
Cutting the cord
Check the vagina for bleeding. If bleeding from the vagina is severe, act quickly. The umbilical cord must be tied because the baby’s blood may be bleeding through the cord and out of the placenta. Tie the umbilical cord six inches from the baby and keep the baby at the same level as the vagina.
If EMS is en route and there is no severe bleeding, do not tie, pinch, or clamp the cord. Place the placenta in a bag or container when it is delivered, and keep it at the same level as the baby.
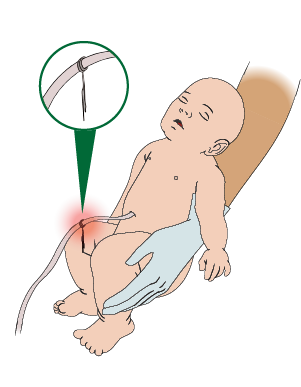
If EMS is delayed or there is severe bleeding:
- Wait until the umbilical cord has stopped pulsating.
- Clamp the cord (or tie with heavy string) 6 and 12 inches from the baby’s body.
- Cut the cord between the clamps with sterile scissors.
Stage 4 – Delivery of the placenta

The placenta usually delivers within 10 to 20 minutes of the birth of the baby. Massaging the lower abdomen can help with the delivery of the placenta, as will nursing.
When the placenta is delivered, wrap it in a plastic bag and ensure it goes to the hospital with the mother and baby.
Complications During Birth
The following are possible complications during the birth.
Newborn is not breathing
In the event that a newborn baby does not start breathing, even after attempting to stimulate them to cry (try for no more than 30 seconds), being CPR.
Provide 30 chest compressions, followed by 2 breaths. Remember that a newborn’s lungs are very small. Use a very small amount of air, just enough for the chest to rise.
Ensure that EMS has been updated. Where possible, have another person provide emotional support for the parents.
Breech birth
A breech birth occurs when a baby does not turn in the womb and delivers with the buttocks emerging first. In this instance, delivery can still progress without serious complications.
To assist during a breech birth:
- Update EMS.
- Support the infant’s body as it is born by placing your arm under the trunk of the body with legs dangling on either side.
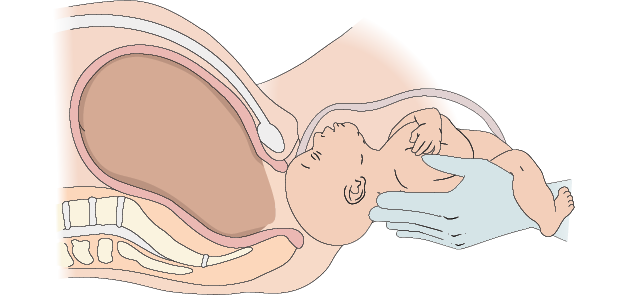
Prolapsed umbilical cord
In some births, the umbilical cord will emerge from the birth canal before the baby. If this happens, do not try to push the umbilical cord back in, and do not pull on it.
Call 9-1-1 again and have the mother avoid pushing.
Limb presentation
In some births, a limb (arm or leg) will deliver before the rest of the baby. This type of birth is very rare and requires an emergency Caesarean section to deliver.
Call 9-1-1 again and update them.
Should this happen, do not pull on the limb. In fact, even touching the presented limb could trigger the baby to begin breathing and suffocate inside the womb.
Multiple births
Multiple births occur when more than one fetus develops in the womb. This can be due to one egg splitting into two fetuses or two eggs being fertilized. This leads to identical or fraternal twins. Multiple births could also be 3 or more.
Some indications that a multiple birth is possible:
- Mother states they are carrying twins (or more)
- Abdomen is still very large after birth of first baby
- Strong contractions begin within 10 minutes of the delivery
- The baby’s size is out of proportion with the size of the mother’s abdomen
The second delivery could occur very soon after the first birth (within a few minutes) or quite some time after (45 minutes or more). In approximately 33% of the cases, the second delivery will be a breech delivery.
 |